 Why do I have spider veins?
Why do I have spider veins?- Do spider veins hurt?
- Do spider veins go away?
- Are spider veins the same as varicose veins?
- How does a doctor treat spider veins?
- What can you do to prevent spider veins?
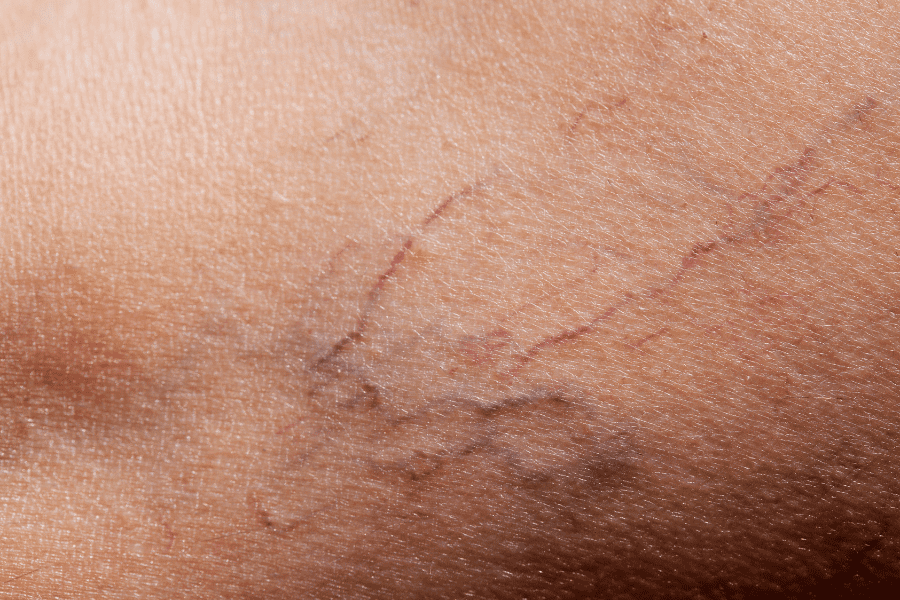
Are you troubled by small red and purple veins just under the surface of your skin? These small lines are called spider veins, a medical condition afflicting the tiny capillaries under the surface of the epidermis, otherwise known as your skin. Spider veins received their nickname by looking like a delicate branching spider web just under the skin’s surface. They are much smaller than engorged varicose veins but can be just as noticeable.
What are spider veins? How do you get them? Can your doctor make them go away? In this article, we’ll go over answers to all of your questions about spider veins and what doctors can do to treat them.
Why Do I Have Spider Veins?
Several factors and lifestyle choices can put you at a greater risk for developing spider veins:
 Exposure to ultraviolet light
Exposure to ultraviolet light- Genetics
- History of blood clots
- Hormones
- Hormone replacement therapy
- Illnesses increase abdominal pressure
- Obesity
- Occupations that require a lot of standing
- Previous vein surgery
- Birth control pills
Women tend to suffer from spider veins more than men. Aging also increases spider vein formation and up to 60% of older adults have the condition.
Medically, spider veins are caused by issues causing abnormal blood flow through veins close to the surface of your skin. To help you understand why this occurs, we’ll briefly cover how the circulatory system functions.
The heart muscle pumps oxygen-rich blood to your organs and extremities. Blood travels along tiny tubes called arteries. When blood circulates through an organ, it is pumped back to the heart through a network of veins. Each vein has a one-way valve that pushes blood toward the heart. Sometimes that valve fails to close properly so the blood can back up and leak into the lower portion of the vein instead of traveling to the heart. That blood becomes stuck and builds up pressure, making the vein bigger and more noticeable. On the skin’s surface, you’ll see the telltale red and blue lines of a spider vein.
Do Spider Veins Hurt?
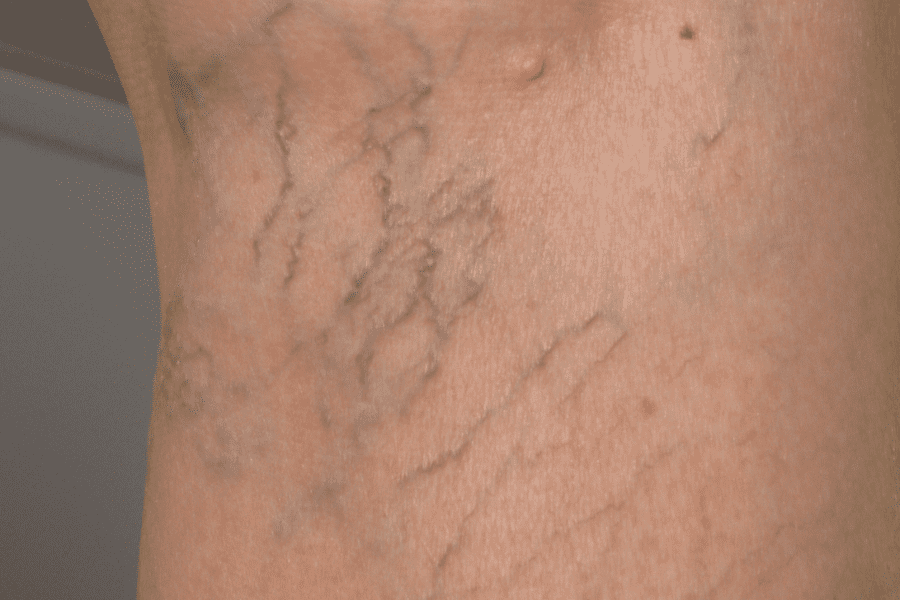 Spider veins can sometimes be painful. The discomfort can worsen over time. Early spider veins may not be uncomfortable at all, but the longer they last, the more you feel cramping or burning can become quite noticeable. Your skin may itch as the red, blue, and purple spider veins become more apparent. Should you see your doctor, or will the spider veins go away on their own?
Spider veins can sometimes be painful. The discomfort can worsen over time. Early spider veins may not be uncomfortable at all, but the longer they last, the more you feel cramping or burning can become quite noticeable. Your skin may itch as the red, blue, and purple spider veins become more apparent. Should you see your doctor, or will the spider veins go away on their own?
Do Spider Veins Go Away?
Spider veins rarely, if ever, go away on their own, but many times they don’t need treatment. While you may be uncomfortable with how they look, spider veins on their own are not threatening. Spider veins on the legs can worsen, particularly if you have a job where you’re on your feet for long periods, or you have a health condition that affects the veins. They can also signal the presence of other vein conditions that are risky to your health.
Spider veins are common in people struggling with weight gain and obesity, which are conditions that often lead to their own set of separate health issues. For example, spider veins may make you more likely to develop varicose veins, which are larger and can occasionally ulcerate, leading to infection. Other vein-related complications include blood clots, which can be life-threatening.
Are Spider Veins the Same as Varicose Veins?
Spider veins are not the same as varicose veins—however, both conditions are caused by vein complications. In appearance, varicose veins look much different than spider veins. By comparison, varicose veins are protrusive, bulging, and swollen. On the other hand, spider veins are more superficial, like light blue or red tracings under the skin that do not change the texture of your skin. Varicose veins also tend to be more painful than spider veins.
How Does a Doctor Treat Spider Veins?
Your doctor may prescribe some self-care treatments to relieve your spider veins, such as resting and elevating the legs after a long day or wearing compression stockings. Compression stockings apply gentle, steady pressure on the area where the spider veins appear. They lessen swelling and keep the blood flowing while reducing your chances of a blood clot.
After a thorough exam, one of the most common treatments for leg veins is a procedure known as sclerotherapy. Sclerotherapy is an effective treatment for eliminating spider veins. The procedure will help by reducing any aches or discomfort that you may feel in the affected area.
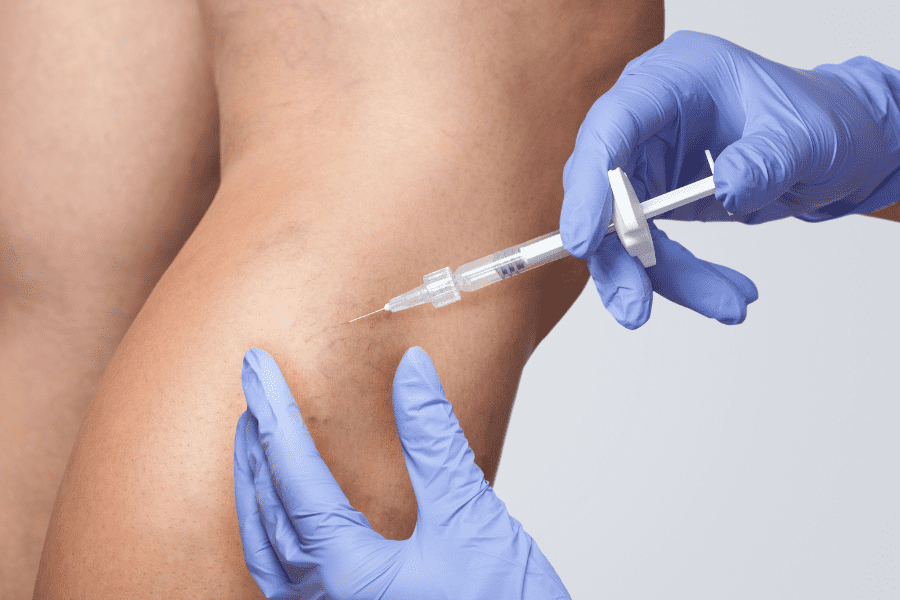 During sclerotherapy, your doctor will:
During sclerotherapy, your doctor will:
- Insert a tiny needle into the spider vein
- Inject a salty chemical solution
- The solution will inflame the vein lining, causing it to swell and tighten
- The doctor will then massage the area to distribute the solution beneath the skin
After the therapy, you will then follow post-procedure protocol by:
- Wearing compression socks for up to three weeks
- The blocked spider veins will slowly reroute to healthier veins
- Over three to six weeks, the spider veins will disappear
Some smaller veins are difficult to treat with sclerotherapy and may require laser therapy. Laser therapy involves placing a laser that heats the vein until it dissolves. During the procedure, you may feel a slight pinching sensation and minimal discomfort. Icing the area after treatment can help relieve any stinging.
Both treatments are very effective at eliminating spider veins. Your doctor will help you determine if these or other treatments can lessen the appearance of your spider veins.
What Can You Do to Prevent Spider Veins?
Although treatment is always an option, you may want to avoid developing spider veins in the first place. Adopting lifestyle changes to prevent spider veins is also useful for patients who undergo treatment since it will help prevent them from recurring.
Here are several methods and lifestyle choices you can follow to minimize your risk of developing spider veins:
- Consider losing weight to help lessen the pressure and weight on your legs
- Exercise regularly to keep blood circulating freely through your heart and extremities
- Stop smoking—not only does smoking hurt your overall health, but it also places unnecessary pressure on your veins and heart
- Wear compression socks and elevate your feet and legs at night
Ultimately, spider veins signal that there may be issues with blood flow in your circulatory system.
Treatment can help. Contact the Vein Care Center of Amelia Island to find out how we can get you back to health.
